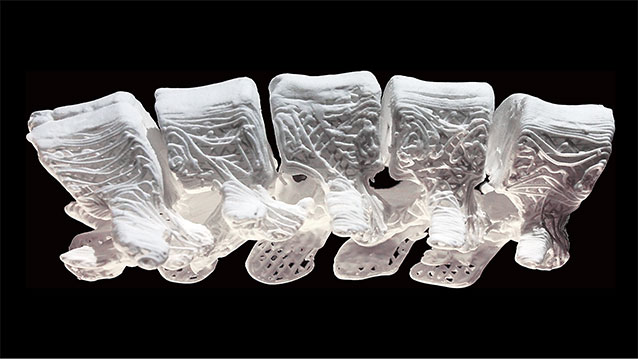
Researchers from the Northwestern University have developed a 3D printable ink that produces a synthetic bone implant that rapidly accelerates bone regeneration and growth.
Image credit: Adam E. Jakus via northwestern.edu
Lead researcher Ramille N. Shah said this hyperelastic “bone” material, which can be easily customised to any desirable shape, could have a massive impact in the treatment of bone defects in children.
“Adults have more options when it comes to implants,” Ms Shah said.
“Paediatric patients do not. If you give them a permanent implant, you have to do more surgeries in the future as they grow. They might face years of difficulty.”
The new 3D printed biomaterial is a mix of hydroxyapatite (a calcium mineral found naturally in human bone) and a biocompatible, biodegradable polymer that is used in many medical applications, including sutures.
Ms Shah said the hyperelastic “bone” material has shown great promise in vivo animal models thanks to its porosity at the nano, micro and macro levels.
“Porosity is huge when it comes to tissue regeneration, because you want cells and blood vessels to infiltrate the scaffold,” she added.
“Our 3D structure has different levels of porosity that is advantageous for its physical and biological properties.”
Hydroxyapatite is known for its ability to induce bone regeneration, but it is also notoriously tricky to work with. Clinical products that use hydroxyapatite are hard and brittle, so previous researchers were forced to create structures composed mostly of polymers, which shields the activity of the bioceramic.
However, this new bone biomaterial is 90% by weight hydroxyapatite and just 10% by weight polymer. Despite its structural composition, the new bone biomaterial still maintains its elasticity because of the way its structure is designed and printed.
Ms Shah said the high concentration of hydroxyapatite creates an environment that induces rapid bone regeneration.
“Cells can sense the hydroxyapatite and respond to its bioactivity,” she added.
“When you put stem cells on our scaffolds, they turn into bone cells and start to up-regulate their expression of bone-specific genes. This is in the absence of any other osteo-inducing substances. It’s just the interaction between the cells and the material itself.”
She said that other substance can also be combined into the ink. Because the 3D printing process is performed at room temperature, the research team was able to incorporate other elements, such as antibiotics, into the ink.
“We can incorporate antibiotics to reduce the possibility of infection after surgery,” Ms Shah said.
“We also can combine the ink with different types of growth factors, if needed, to further enhance regeneration. It’s really a multi-functional material.”
The biggest advantage that the new bone biomaterial has to offer is that it will allow the end product to be customised to the patient. Using Ms Shah’s synthetic material, physicians will now be able to scan the patient’s body and 3D print a personalised product. Additionally, the biomaterial also can be easily trimmed and cut to size and shape during a procedure.
“The turnaround time for an implant that’s specialized for a customer could be within 24 hours,” she said.
“That could change the world of craniofacial and orthopaedic surgery, and, I hope, will improve patient outcomes.”



















